
Simplify Care Management in a Value-Based Care Setting with Rising Risk
Streamline your organization’s workflow and improve patient outcomes today.
UConn Health achieves success while using Rising Risk
In this video, Khadija Poitras-Rhea, Assistant VP of Population Health, discusses UConn Health’s recent experience leveraging the Rising Risk solution to easily coordinate post-discharge patient workflow and increase their ability to identify emerging high-risk patients within their clinical workflows.
One of their goals in using our Rising Risk solution was to help identify UConn Health’s recurring Emergency Department high utilizers and try to get those patients reconnected with their primary care provider to close the gaps in care and provide better transitional care management.
The results were astounding. UConn Health increased their transitional care management capture rate by 300%, which helped significantly increase the quality of care for the patients and generate more revenue for the organization.
Listen to Khadija’s story by watching the video below.
Speak to a Bamboo Health Expert
Find out how Rising Risk can help streamline your organization’s workflow and improve patient outcomes.
Thank you for filling out our form. Someone will reach out to you soon!


Efficient care and cost savings
Did you know that patients with multiple severe and chronic conditions have an elevated risk of high-cost care? Care coordinators must often wait 60-90 days for claims data to identify the high-risk patient population, resulting in delayed care opportunities, increased operational costs, and poor patient outcomes.
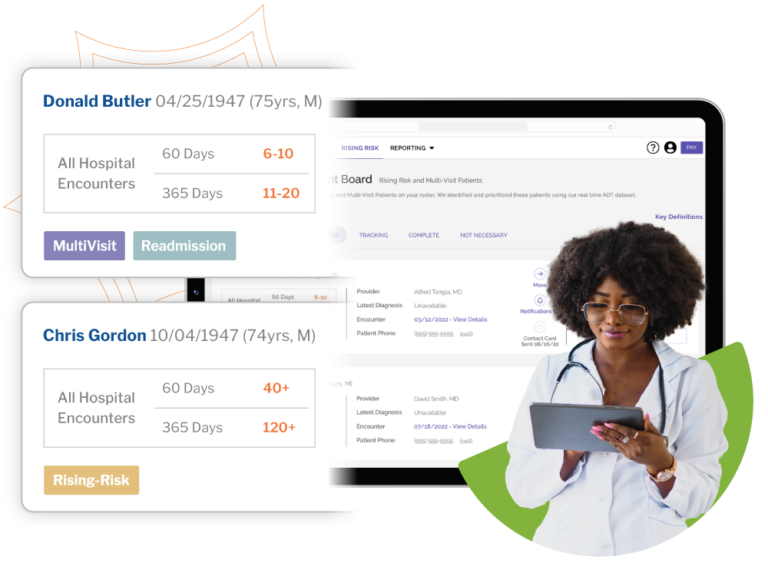
Powered by real-time data and analytics
Rising Risk provides care managers and physicians with an effective post-discharge follow-up workflow for prioritized patients. This helps reduce recurring ED visits and eliminate unnecessary costs, thus, improving the patient’s overall outcomes and quality of care.

During the very first phone call, the Nurse Care Manager contacted the patient to enroll in care management and talk about a care plan and the patient was actually laying on the floor because she had fallen and couldn’t get up. That phone call would not have happened if not for the patient showing up on her Rising Risk list that morning.
Khadija Poitras-Rhea, LCSW Assistant VP of Population Health, UConn Health
Contact Us.
Find out how Rising Risk can help streamline your organization’s workflow and improve patient outcomes by speaking to one of our Bamboo Health experts.
Contact an Expert