
Rising Risk
High-Risk Patient Identification & Care Management Platform
Rising Risk proactively identifies high-risk patients who may be missed by traditional stratification models, enabling care teams to quickly prioritize and intervene, resulting in improved outcomes and cost savings.

Drive Better Outcomes
Provider organizations must identify high-risk patients for timely intervention, but relying on claims data can delay the process, resulting in poor quality of patient care, high costs and reduced reimbursement.
Rising Risk helps healthcare provider organizations and professionals identify, prioritize and engage the high-risk patients who are most likely to benefit from the intervention of a care management team. Considering care events as well as social determinants of health, Rising Risk helps providers remove previous barriers to care, improve the patient experience and drive better outcomes.
Key Benefits
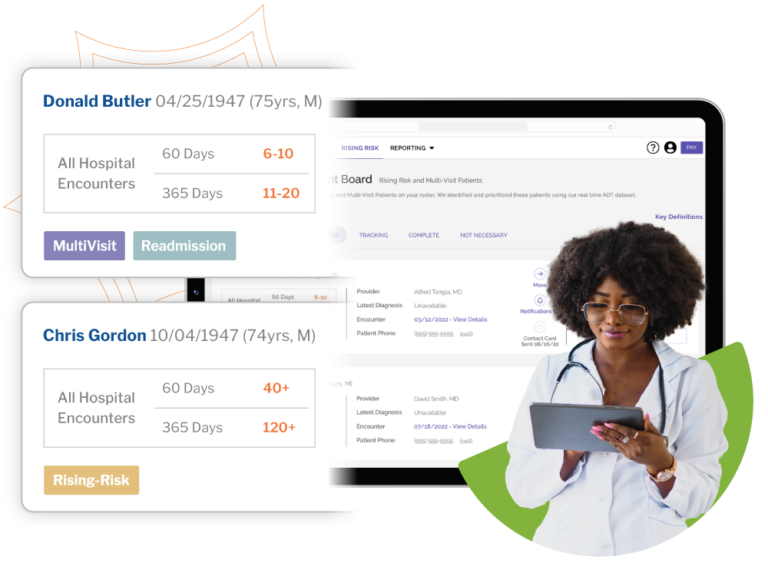
Improve Speed & Accuracy
The innovative risk scoring model leverages Bamboo Health’s nationwide, real-time admission, discharge and transfer (ADT) network, driving utilization awareness and increasing care management program enrollment.


Drive Care Management Team Alignment
Rising Risk goes beyond being a patient risk solution, providing real-time intelligence and analytics and workflow features that enable more informed decision making and collaborative care.
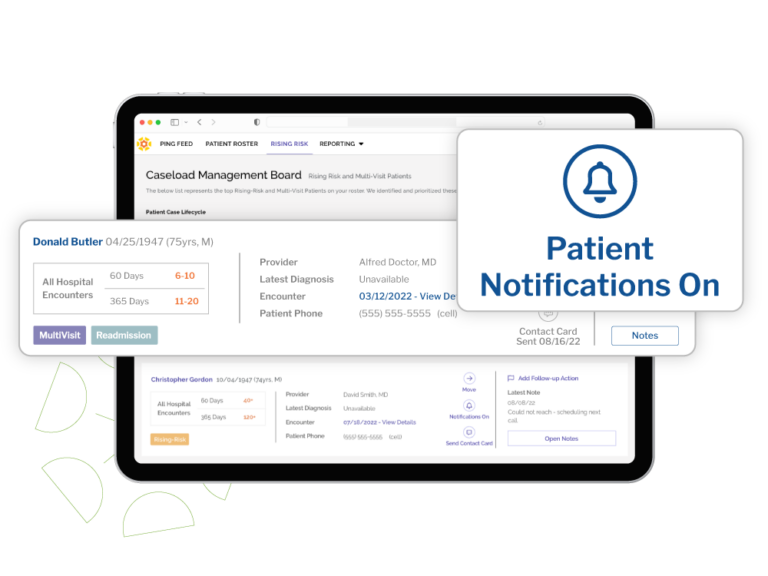
Increase Patient Engagement
Care team members can more actively engage hard-to-reach patients for important follow-up care using Rising Risk’s user-friendly interface and in-app workflow tools.

Our Impact
Rising Risk helps hospitals, payers, ACOs and post-acute providers create smoother transitions of care for high-risk patient populations and improve both clinical and financial outcomes
Learn More-
50%
reduction in cost of multi-visit patients
-
1B+
patient encounters per year
Featured Resources
View More InsightsGet in Touch
Speak with Us
Tell us all about your organization’s care coordination and care intelligence needs.
Speak with Us
Schedule a Demo
See how our technologies deliver critical patient information in real-time and in clinical workflows.
Schedule a Demo
View Our Resources
Read more about our customers’ successes and how we’re working to improve public health.
View Our Resources





